HISTORY 135F

Infectious and
Epidemic Disease in History
Department of History
University of California, Irvine
Instructor: Dr. Barbara J. Becker
HISTORY 135F

Infectious and
Epidemic Disease in History
Department of History
University of California, Irvine
Instructor: Dr. Barbara J. Becker
|
Three employees at Behringwerke AG, a virus-production facility, fall sick
Victims shared one common factor--contact with African green monkeys |
|
|
Cells from kidneys of green monkeys:
Employees at Behring were harvesting monkey kidney cells for production of polio virus vaccine. The green monkeys being used in this procedure were:
|
|
Subsequent tests on guinea pigs turned up an organism that no one had ever seen before--family of viruses now called the Filoviridae ... |
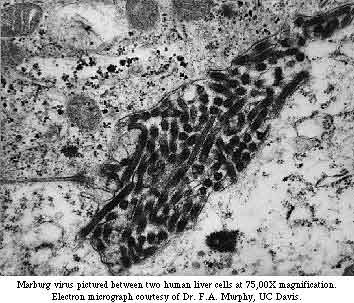 |
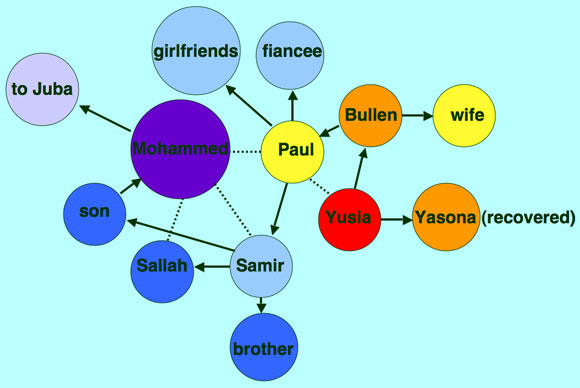
June 1976 June 27--Yusia falls sick
July 2--Yusia's symptoms worsen
July 13--Yasona becomes sick (eventually recovers!) July 12--Bullen, storekeeper from cotton factory becomes ill
July 14--Bullen dies
August 18--Sallah becomes sick and dies; as does one of Mohammed's sons August 21--Mohammed becomes sick
Epidemiologists later trace 48 cases of illness and 27 deaths to contact with Paul. |
Yambuku, Zaire (now Democratic
Republic of the Congo [DRC])
August, 1976 (Belgian Catholic Mission Hospital in Yambuku services 60,000 villagers in central Bumba Zone) |
|||
|
August 12-22
August 30--despite deteriorating health, man discharges himself from hospital
September 17--he issues first official report
of the events
Early October--team of medical experts arrives in Yambuku
|
|
The infecting agent in the Yambuku epidemic was identified as a virus, another of the filoviridae. It was named Ebola, after the Congo's Ebola River, where it was believed to have originated. Comparison of the viruses responsible for the disease outbreaks in Sudan and Zaire revealed them to be distinct strains of ebola virus. Of the two, ebola Zaire was the more virulent. In 1989, third strain was discovered during an outbreak among monkeys in a research laboratory in Reston, Virginia. No humans became sick from their exposure to this strain although some did develop antibodies to it. In 1995, a fourth strain was found. Chimpanzees in the Tai Forest, Ivory Coast, died of this strain. One researcher studying this outbreak became ill, but recovered. |
|
|
|
|
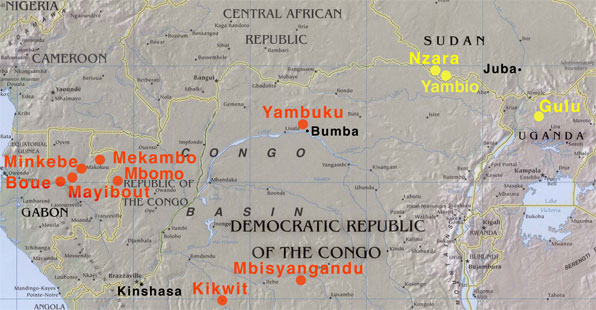
| June 1976 | · Nzara, Sudan |
|
| August 1976 | · Yambuku, Zaire (now Democratic Republic of the Congo [DRC]) |
|
| 1979 | · Nzara, Sudan |
|
| 1989 and 1990 | · Reston, Virginia
(also found in other animal research facilities in Texas and Pennsylvania) |
|
| 1992 | · Siena, Italy | *see comments above |
| 1994 | · Minkebe, Gabon |
|
| 1995 | · Kikwit, DRC |
|
| 1996 | · Mayibout, Gabon
· Boue, Gabon |
60 (45) |
| · Alice, Texas
· Philippines |
*see comments above |
|
| 2000-2001 | · Gulu, Uganda |
|
Patients receive care at Lacor Hospital in Gulu.
Corpses of ebola victims are handled with great care...
...to prevent the virus from spreading.
Bodies are placed in graves by staff wearing protective clothing. |
||
| 2001-2002 | · Mbisyangandu, DRC |
|
| · Mekambo, Gabon |
|
|
| 2003 | · Mbomo, Rep. of Congo | |
| 2004 | · Yambio, Sudan | |
| 2005 | · Mbomo, Rep. of Congo | |
 |
| Go to: |
|
|